
I am hoping to be selected for the Health eVoice 2020 conference.
This would be such an honor.
Here is a short video
Thank you.

I am hoping to be selected for the Health eVoice 2020 conference.
This would be such an honor.
Here is a short video
Thank you.

Wow I am beyond honored I’ve now also been
Nominated for Patient Leader Hero- Healthcare Collaborator – Rookie of The Year and Best In Show Blog
Endorsements Now Open If You Would Like to Vote (link below)
I have been nominated for the past few years in various categories
Thank You for considering Endorsing my nominations
It’s deeply appreciated
Thank You
Your hips are largest and most powerful of muscle groups—the glutes, quads, and hamstrings—all connect at the hips, and they allow you to walk, run, climb. The hip joint is crucial to all movement, in sports and day-to-day life, which is why persistent hip pain can be such a pain in the ass literally and often debilitating.

Wear and tear on your hip joint can worsen with age. According to the Centers for Disease Control and Prevention, 7 percent of adults in the U.S. suffer from hip pain, the third most common joint pain behind shoulder pain, at 9 percent, and knee pain, at 18 percent. There’s also a growing prevalence of young athletes with hip injuries, especially young women, due to repetitive overuse and acute trauma.
Trauma can sometimes lead to osteonecrosis in any joint but we are focusing on the hip , and some of the medications given to help inflammation and strengthen bones can also be a cause of osteonecrosis aka avascular necrosis.
Your Hip Pain May be the Sign of a Rare Condition
If you have hip pain don’t always brush it off as arthritis, if it persists, get it checked out to be safe
Persistent or worsening hip pain warrants a visit to your health care provider and possibly a sports medicine specialist or ortho. Some problems, particularly hip stress fractures, are commonly misdiagnosed due to the confusing presentation of symptoms.
A thorough evaluation is necessary and often includes X-rays and other studies, such as an MRI or bone scan. As with all injuries, the absence of pain does not mean that all is well. Strength and flexibility deficits must be addressed to allow a healthy return to helping your quality of life.
Although a person may not initially experience symptoms, hip pain is usually the first indicator. The earlier the diagnosis is achieved, the better the patient’s potential outcome. AVN has four stages that can progress over a period of several months to more than a year. In Stage I, the hip is healthy; in Stage II, the patient experiences mild to moderate pain in direct proportion to the deterioration of the head of the femur (or ball of the hip joint). By Stage III, usually the patient will find it difficult to stand and bear weight on the hip, and joint movement will be painful. During this stage, the ball of the hip has deteriorated to what is called a subchondral fracture and early collapse. Stage IV is a full collapse of the femoral head and degenerative joint disease (DJD).
Treatment for AVN is recommended based on the stage of the disease coupled with the age of the patient. In Stage I, medication and crutches may be prescribed to provide relief and enable the bone to heal on its own. This treatment may require the patient to be non-weight-bearing for up to six months. It also has a failure rate greater than 80-percent.
On the horizon treatments are stem cell.
Surgical treatment is recommended with a Stage II diagnosis, or very early in a Stage III diagnosis. A procedure, known as a core decompression, typically involves drilling one large hole in the core of the effected bone, with or without a bone graft, to reduced pressure and improve blood circulation in the hip. Another surgical option is the vascularized fibular graft, which takes a healthy piece of bone from the fibula, along with the artery or vein, and transplants and reattaches it into the hip, to help healthy bone grow. Recovery can take several months.
Because most patients are diagnosed in late Stage III or IV of the disease, when the bone quality of the femoral head is poor (subchondral fracture) or has collapsed, total hip replacement is the most successful treatment for AVN. This procedure replaces the damaged bone with artificial parts. Recovery takes about eight to twelve weeks. If left untreated, AVN progresses and results in pain and severe debilitating osteoarthritis.
Treatment decisions for AVN are ultimately up to the patient and are based on his or her lifestyle and goals. If you are suffering with hip pain, talk with your primary care doctor about a referral to an orthopedic surgeon
Osteonecrosis of the Hip
Osteonecrosis of the hip is a painful condition that occurs when the blood supply to the head of the femur (thighbone) is disrupted. Because bone cells need a steady supply of blood to stay healthy, osteonecrosis can ultimately lead to destruction of the hip joint and severe arthritis.
Osteonecrosis is also called avascular necrosis (AVN) or aseptic necrosis. Although it can occur in any bone, osteonecrosis most often affects the hip. More than 20,000 people each year enter hospitals for treatment of osteonecrosis of the hip. In many cases, both hips are affected by the disease.
After discussing your symptoms and medical history, your doctor will examine your hip to discover which specific motions cause your pain.
Patients with osteonecrosis often have severe pain in the hip joint but relatively good range of motion. This is because only the femoral head is involved in the earlier stages of the disease. Later, as the surface of the femoral head collapses, the entire joint becomes arthritic. Loss of motion and stiffness can then develop.
Osteonecrosis is typically seen as a wedge-shaped area with a dense whitish sclerotic border in the superior lateral portion of the femoral head. On lateral view, a lucent line called a “crescent sign” can often be seen just below the surface of the femoral head.
Magnetic resonance imaging (MRI) scans.Early changes in the bone that may not show up on an x-ray can be detected with an MRI scan. These scans are used to evaluate how much of the bone is affected by the disease. An MRI may also show early osteonecrosis that has yet to cause symptoms (for example — osteonecrosis that may be developing in the opposite hip joint).
Stages of Avascular Necrosis-Osteonecrosis Hip
photo credit AAOS American Academy of Orthopaedic Surgeons

Video Link of Stages of Avascular Necrosis-Osteonecrosis Hip
Dr Nabil Ebraheim Shows Info on Hip Avascular Necrosis
You can have Avascular Necrosis in one hip or both , if in both hips it’s called bilateral which means both sides.
And if you have Avascular Necrosis- osteonecrosis in more that 3 different joints
Multifocal osteonecrosis is defined as disease involving three or more anatomic sites.
Example
Hips
Knees
Shoulder
That is called multi focal Avascular Necrosis- Osteonecrosis
Read more
Multifocal osteonecrosis Article in The Journal of Rheumatology 25(10):1968-74 · November 1998
Multifocal ON, which ON involves three or more distinct anatomical sites [5], is rare, being seen in only approximately 3% of all ON patients [5]. Corticosteroid use is a known risk factor for multifocal ON [5,6], as are certain comorbidities, including systemic lupus erythematosus (SLE), renal failure, leukemia, and lymphoma [5,7,8]. However, almost all studies of multifocal ON are case reports and case series, so the inci- dence and clinical characteristics of the condition remain poorly defined [5,[8][9][10][11][12][13]. …
Non-operative Treatment
There is no known pharmaceutical cure for osteonecrosis. Several non-operative treatments have been studied including hyperbaric oxygen therapy, shock wave therapy, electrical stimulation, pharmaceuticals (anticoagulants, bisphosphonates, vasodilators, lipid lowering agents), physiotherapy and muscle strengthening exercises, and combinations thereof. There are conflicting results for some of these treatments, therefore, rigorous, randomized controlled trials with large numbers of patients are still needed to determine the effectiveness of these treatments. Non-operative treatment may be part of a wait-and-see approach based on the size of the area of dead bone. Non-operative treatments cannot be labeled as conservative, since many of them do not slow the progression of the disease or lead to avoidance of a total hip arthroplasty. Most are simply pain-relieving at best.
Reduced weight bearing does not alter the course of the disease and is not a treatment. It may be used to simply permit the patient to better cope with pain until appropriate treatment is instituted.
Surgical Treatment
Core decompression – This surgical procedure removes or drills a tunnel into the area of the affected bone, which reduces pressure within the bone. Core decompression works best in people who are in the earliest stages of osteonecrosis, before the collapse of the dead bone. This procedure sometimes can reduce pain and slow the progression of bone and joint destruction in these patients.
Osteotomy – This surgical procedure reshapes the bone to reduce stress on the affected area. There is a lengthy recovery period, and the patient’s activities are very limited for 3 to 12 months after an osteotomy. This procedure is most effective for patients with advanced osteonecrosis and those with a small area of affected bone.
Bone graft – Bone grafts can be used as part of the surgical treatment for osteonecrosis. Bone grafts can use bone from the same patient or donor bone. Bone graft or synthetic bone graft can be inserted into the hole created by the core decompression procedure. A specialized procedure, called vascularized bone grafting, involves moving a piece of bone from another site (often the fibula, one of the bones of the calf, or the iliac crest, a portion of the pelvic bone) with a vascular attachment. This allows for support of the diseased area as well as a new source of blood supply. This is a complex procedure and is performed by surgeons that are specially trained. Another type of bone grafting, involves scraping out all of the dead bone and replacing it with healthier bone graft, often from other portions of the patient’s skeleton.
A unique type of bone graft involves the use of a patient’s own cells that are capable of making new bone. Often these cells are a type of stem cell from the bone marrow or other bodily tissues. There has been increasing interest in the potential of stem cell therapy. This is also being studied for the treatment of osteonecrosis. Mesenchymal stem cells, which are a type of ‘adult’ stem cell, can grow and develop into many different cell types in the body. Physicians take the patient’s own mesenchymal stem cells (autologous transplant) and place them into the affected bone to stimulate bone repair and regeneration.
Arthroplasty/total joint replacement – Total joint replacement is the treatment of choice in late-stage osteonecrosis when the joint is destroyed. In this surgery, the diseased joint is replaced with artificial parts. It may be recommended for people who are not good candidates for other treatments, such as patients who do not do well with repeated attempts to preserve the joint. Various types of replacements are available, and people should discuss specific needs with their doctor.
For most people with osteonecrosis, treatment is an ongoing process. Doctors may first recommend the least complex and invasive procedure, such as protecting the joint by limiting high impact activities, and watch the effect on the patient’s condition.
Other treatments then may be used to prevent further bone destruction and reduce pain such as core decompression with bone graft/stem cell therapy. Eventually patients may need joint replacement if the disease has progressed to collapse of the bone. It is important that patients carefully follow instructions about activity limitations and work closely with their doctor to ensure that appropriate treatments are used.
Scientists, researchers, and physicians continue to pursue a better understanding of how this disease occurs as well as compare the effectiveness of current and newly developed therapies. Often, this requires a clinical trial to answer questions and gain additional knowledge.
Information on current clinical trials is posted on the Internet at www.clinicaltrials.gov. All studies receiving U.S. government funding, and some supported by private industry, are posted on this government web site.
For information about clinical trials being conducted at the NIH Clinical Center in Bethesda, MD, contact the NIH Patient Recruitment Office:
Toll-free: (800) 411-1222
TTY: (866) 411-1010
Email: prpl@cc.nih.gov
Nontraumatic Osteonecrosis of the Femoral Head: Where Do We Stand Today? A Ten-Year Update.
By Dr. Michal Mont MD
The goal is to prevent further bone loss.
In the early stages of avascular necrosis, symptoms might be eased with medication and therapy. Your doctor might recommend:
Because most people don’t develop symptoms until avascular necrosis is fairly advanced, your doctor might recommend surgery. The options include:
Talk to your doctor about treatment options and the stage of your Avascular Necrosis of the Hip.
If this helped you please like comment or share this.
Thank You
Wishing you a pain free day
Debbie
We are #rare!!
Celebrate You’re Rare
Facts
Osteonecrosis – Avascular Necrosis -Aseptic Necrosis-Ischemic Necrosis-Bone Infarction- has many different names and causes.In children its Legg Calves Perthes.
They all mean – A Loss of blood supply to the bone which may lead to bone cell death and can be caused by an injury (meniscal tear -bone fracture or joint dislocation; called traumatic osteonecrosis).
There may be no history of injury (non-traumatic osteonecrosis); however, other risk factors are associated with the disease such as some medications (steroids, also known as corticosteroids), alcohol usage or blood coagulation disorders. Increased pressure within the bone also is associated with osteonecrosis.
One theory is that the pressure within the bone causes the blood vessels to narrow, making it difficult for blood to circulate through the bone. Osteonecrosis can also be associated with other disorders. The exact reason osteonecrosis develops is not fully understood for some risk factors.

Sometimes, osteonecrosis occurs in people with no risk factors (idiopathic). Some people have multiple risk factors. Osteonecrosis most likely develops because of the combination of factors, possibly including genetic, metabolic, self-imposed (alcohol, smoking), and other diseases that you may have and their treatment.
Injury:
When a joint any joint hip,knee, shoulder, ankle, elbow is injured, as in a fracture or dislocation, meniscus tear the blood vessels may be damaged.
This can interfere with the blood circulation to the bone and lead to trauma-related osteonecrosis.
Studies suggest that this type of osteonecrosis may develop in more than 20% of people who dislocate their hip joint.
Corticosteroid Medications:
Corticosteroids, such as prednisone, are commonly used to treat diseases in which there is inflammation, such as systemic lupus erythematosus, rheumatoid arthritis, inflammatory bowel disease, and vasculitis. Studies suggest that long-term, high dose systemic (oral or intravenous) corticosteroid use is a major risk factor for non-traumatic osteonecrosis with reports of up to 35 percent of all people with non-traumatic osteonecrosis.
And corticosteroids come in many versions – inhaled and ingested corticosteroids for asthma-cold-sinus problems or steroid injections into joints, topical for skin-
Patients should discuss concerns about corticosteroid use with their doctor.
Doctors aren’t sure exactly why the use of corticosteroids sometimes is associated with osteonecrosis. They may have negative effects on different organs and tissues within the body. For example, they may interfere with the body’s ability to build new bones and to break down fatty substances.
These substances would then build up in and clog the blood vessels, causing them to narrow. This then would reduce the ability of blood to flow inside a bone.
Alcohol Use:
Excessive alcohol use is another major risk factor for non-traumatic osteonecrosis. Studies have reported that alcohol accounts for about 30% of all people with non-traumatic osteonecrosis. While alcohol can slow down bone remodeling (the balance between forming new bone and removing bone), it is not known why or how alcohol can trigger osteonecrosis.
Other Risk Factors:
Other risk factors or conditions associated with non-traumatic osteonecrosis include Gaucher disease, pancreatitis, autoimmune disease, cancer, HIV infection, decompression disease (Caisson disease), and blood disorders such as sickle cell disease. Certain medical treatments including radiation treatments and chemotherapy can cause osteonecrosis. People who have received a kidney or other organ transplant may also have an increased risk.
Affected Populations
Osteonecrosis usually affects people between 30 and 50 years of age; about 10,000 to 20,000 people develop osteonecrosis each year in the United States.
Osteonecrosis affects both men and women and affects people of all ages. It is most common among people in their thirties and forties.
Depending on a person’s risk factors and whether the underlying cause is trauma, it also can affect younger or older people.
Related Disorders
Some Symptoms of the disorders listed below may be similar to those of osteonecrosis. Comparisons may be useful for a differential diagnosis:
Osteopetrosis is a combination of several rare genetically caused symptoms grouped together as one disorder. It can be inherited and is marked by increased bone density, brittle bones, and, in some people, skeletal abnormalities. Although symptoms may not initially be apparent to people with mild forms of this disorder, trivial injuries may cause bone fractures due to abnormalities of the bone. The dominantly transmitted form is milder than the recessive form and may not be diagnosed until adolescence or adulthood when symptoms first appear. More serious complications occur in the recessive form which may be diagnosed from examination of skeletal x-rays during infancy or childhood. (For more information on this disorder, choose “Osteopetrosis” as your search term in the Rare Disease Database.)
Reflex sympathetic dystrophy syndrome (RSDS), also known as complex regional pain syndrome, is a rare disorder of the sympathetic nervous system that is characterized by chronic and severe pain. The sympathetic nervous system is that part of the autonomic nervous system that regulates involuntary functions of the body such as increasing heart rate, constricting blood vessels, and increasing blood pressure. Excessive or abnormal responses of portions of the sympathetic nervous system are thought to be responsible for the pain associated with reflex sympathetic dystrophy syndrome. The symptoms of RSDS typically begin with burning pain, especially in an arm, finger(s), palm of the hand(s), and/or shoulder(s). In some individuals, RSDS may occur in one or both legs or it may be localized to one knee or hip. Frequently, RSDS may be misdiagnosed as a painful nerve injury. The skin over the affected area(s) may become swollen (edema) and inflamed. Affected skin may be extremely sensitive to touch and to hot or cold temperatures (cutaneous hypersensitivity). The affected limb(s) may perspire excessively and be warm to the touch (vasomotor instability). The exact cause of RSDS is not fully understood, although it may be associated with injury to the nerves, trauma, surgery, atherosclerotic cardiovascular disease, infection, or radiation therapy. (For more information on this disorder, choose “reflex sympathetic dystrophy” as your search term in the Rare Disease Database.)
Legg-Calvé-Perthes disease (LCPD) is one of a group of disorders known as the osteochondroses. The osteochondroses typically are characterized by degeneration and subsequent regeneration of the growing end of a bone (epiphyses). In LCPD, the growing end of the upper portion of the thigh bone (femur) is affected. The upper section of the thigh bone is known as the head or “the ball” and connects to the hip in a depression or “socket”. This is the hip joint, which is a ball and socket joint. The disorder results from an unexplained interruption of the blood supply (ischemia) to the head of the femur, which causes degeneration and deformity of the femoral head. Symptoms may include a limp with or without pain in the hip, knee, thigh, and/or groin; muscle spasms; and/or limited or restricted movement of the affected hip. The disease process seems to be self-limiting as new blood supplies are established (revascularization) and new healthy bone forms (re-ossifies) in the affected area. The exact cause for the temporary interruption of blood flow to the femoral epiphysis is not fully understood. Most times the disorder appears to occur randomly for no apparent reason (sporadically).
#RareDiseaseDay2019February28
#RareDiseaseDay
#CelebrateYourRare
#Awareness #Education
Osteonecrosis-Avascular Necrosis -Broken Down
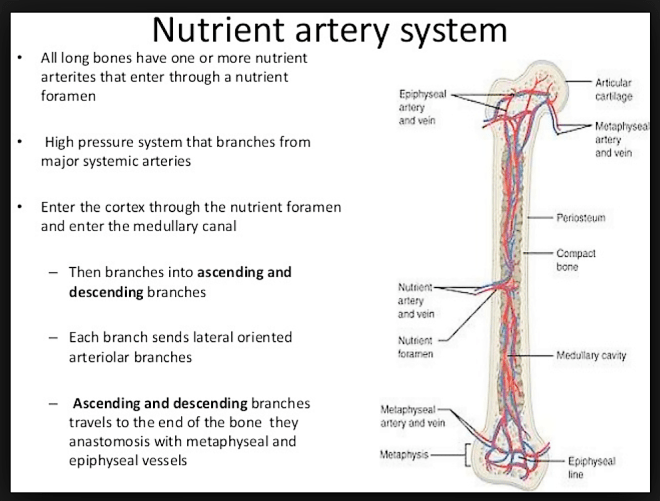
Osteonecrosis is the death of a segment of bone caused by an impaired blood supply. We all need an adequate blood supply to the bone other wise the bone can collapse and die. The blood supply to bone is delivered to the endosteal cavity by nutrient arteries, then flows through marrow sinusoids before exiting via numerous small vessels that ramify through the cortex. Reductions in vascular supply are associated with bone loss. Bones in our body are living tissue. They have their own blood vessels and are made of living cells, which help them to grow and to repair themselves. As well, proteins, minerals and vitamins make up the bone when you get to little blood flow the bone breaksdown much faster than it can repair and generate new bone.
This disorder can be caused by an injury or can occur spontaneously.
Typical symptoms include pain, limited range of motion of the affected joint, and, when the leg is affected, a limp.
The diagnosis is based on symptoms, the person’s risk of osteonecrosis, and the results of x-rays and magnetic resonance imaging.
Stopping smoking, stopping excessive alcohol use, and minimizing the use of or lowering the dose of corticosteroids reduce the risk of developing the disorder.
Various surgical procedures can be done if nonsurgical measures (such as rest, physical therapy, and pain relievers) do not relieve symptoms. Eat a healthy diet
Each year in the United States, about 20,000 people develop osteonecrosis. The hip is most commonly affected, followed by the knee and shoulder. The wrist and ankle are affected less often. Osteonecrosis does not usually affect the shoulder or other less commonly affected sites unless the hip is also affected. However, osteonecrosis of the jaw (ONJ) is a disorder involving only the jaw bone.
Causes
Osteonecrosis is not a specific disease but a condition in which death of the bone is confined to one or more specific (localized) areas. There are two general categories of osteonecrosis:Making it a rare disorder.
Traumatic (following an injury)
Nontraumatic
Traumatic osteonecrosis is the most common. The most frequent cause of traumatic osteonecrosis is a displaced fracture. In a displaced fracture, a bone breaks into two or more parts and moves so that the fractured ends are not lined up. The type of displaced fracture that causes osteonecrosis most often affects the hip (see Hip Fractures) and most commonly occurs in older people.
Another cause of traumatic osteonecrosis is a dislocation. A dislocation occurs when the ends of bones in joints become completely separated from each other, as in a hip dislocation.
A displaced fracture or a dislocation may damage the blood vessels supplying the upper end of the thighbone (the femoral head, part of the hip joint), resulting in death of this part of the bone. This death of bone occurs less often in other areas of the body.
Some Risk Factors for Osteonecrosis
Traumatic osteonecrosis- injury to bone or joint like meniscal tear -broken bones-dislocations etc…
Fractures (breaks in bones) and dislocations (when the ends of bones in joints become completely separated from each other)
Nontraumatic osteonecrosis
Excessive alcohol
Blood clotting (coagulation) disorders
Bone Marrow Edema
Chemotherapy
Corticosteroids
Cushing syndrome
Decompression sickness
Gaucher disease
High level of lipids in the blood (hyperlipidemia)
HIV infection
Liver disease
Lupus and other autoimmune connective tissue disorders
Miscellaneous conditions (such as chronic kidney disease and rare genetic mutations)
Organ transplantation
Pancreatitis
Radiation
Sickle cell disease
Smoking
Tumors
Vasculitis
Nontraumatic osteonecrosis occurs without direct trauma or injury. This type may be caused by a disease or condition that results in the blockage of small blood vessels that supply certain areas of the bone. The areas most commonly affected are the femoral head (which is part of the hip joint), the knee, and the upper arm at the shoulder. This disorder occurs most commonly among men and people between the ages of 30 and 50 and often affects both hips or both shoulders. The most common causes are
Corticosteroids (when given at high doses, for long periods of time, or both)
Chronic, excessive alcohol use (more than 3 drinks a day for several years)
A number of other causes have been identified, but these occur much less often. These other causes include certain blood-clotting disorders, sickle cell disease, liver disease, tumors, Gaucher disease, radiation therapy, and decompression sickness (which occurs in divers who surface too quickly). A number of disorders that are treated with high doses of corticosteroids (such as lupus) also may be associated with osteonecrosis. In these cases, it may not be clear whether the cause is the disorder or the corticosteroids.
In about 20% of people with osteonecrosis, the cause is unknown.
If one bone has nontraumatic osteonecrosis, the same bone on the opposite side of the body sometimes has it also, even if there are no symptoms. For example, if one hip is affected, about 60% of the time the other hip is affected.
Spontaneous osteonecrosis of the knee (SPONK or SONK) can occur in older women (occasionally men) who have no specific risk factors for the disorder. SPONK differs from other forms of osteonecrosis. SPONK is thought to be caused by an insufficiency fracture. An insufficiency fracture is caused by normal wear and tear on bone that has been affected by osteoporosis. SPONK occurs without direct trauma or injury.
Symptoms
As osteonecrosis progresses, more and more tiny fractures may occur, particularly in bones that support weight, such as the hip. As a result, the bone usually collapses weeks or months after the blood supply is cut off. Most often pain develops gradually when the bone begins to collapse. At times, however, pain may begin suddenly and could be related to increased pressure that develops in and around the affected area of bone. Regardless of how sudden, pain is increased by moving the affected bone and typically is alleviated with rest. The person avoids moving the joint to minimize pain.
If the affected bone is in the leg, standing or walking worsens the pain and a limp develops.
In osteonecrosis of the hip, pain is usually present in the groin and may extend down the thigh or into the buttocks.
Spontaneous osteonecrosis of the knee causes sudden pain along the inner part of the knee. There may be tenderness in this area, and the joint often becomes swollen with excess fluid. Bending the knee may be painful, and people may have a limp.
Osteonecrosis of the shoulder often causes fewer symptoms than osteonecrosis that occurs in the hip or knee.
Osteoarthritis (damage to the cartilage covering the joint surfaces) develops over time, often after a large part of the bone collapses.
Diagnosis
X-rays
Magnetic resonance imaging
Because osteonecrosis is often painless at first, it may not be diagnosed in its earliest stages. Doctors suspect osteonecrosis in people who do not improve satisfactorily after having certain fractures. They also suspect the disorder in people who develop unexplained pain in the hip, knee, or shoulder, particularly if these people have risk factors for osteonecrosis.
X-rays of the affected area usually show osteonecrosis unless the disorder is in its earliest stages. If x-rays appear normal, however, magnetic resonance imaging (MRI) is usually done because it is the best test for detecting osteonecrosis early, before changes appear on ordinary x-rays. The x-rays and MRI also show whether the bone has collapsed, how advanced the disorder is, and whether the joint is affected by osteoarthritis. If doctors discover nontraumatic osteonecrosis in one hip, they also examine the other hip with an x-ray or MRI.
Blood tests may be done to detect an underlying disorder (such as a blood-clotting disorder).
Prevention
To minimize the risk of osteonecrosis caused by corticosteroids, doctors use these drugs only when essential, prescribe them in as low a dose as needed, and prescribe them for as short a duration as possible.
To prevent osteonecrosis caused by decompression sickness, people should follow accepted rules for decompression during diving and when working in pressurized environments (see prevention of decompression sickness and see Diving Safety Precautions and Prevention of Diving Injuries).
Excessive alcohol use and smoking should be avoided.
Various drugs (such as those that prevent blood clots, dilate blood vessels, or lower lipid levels) are being evaluated for prevention of osteonecrosis in people at high risk.
Treatment
Nonsurgical measures to relieve symptoms
Surgical procedures
Hip replacement
Some areas affected by osteonecrosis need only nonsurgical measures to relieve symptoms. Other areas need to be treated with a surgical procedure.
Nonsurgical measures
Several nonsurgical measures are available for treating the symptoms caused by osteonecrosis. Taking anti-inflammatory drugs or other pain relievers, minimizing activity and stress (such as weight bearing for osteonecrosis of the hip and knee), and undergoing physical therapy are ways to relieve symptoms but not cure the disorder or change its course. These measures, however, may be adequate for treatment of the shoulder, the knee, spontaneous osteonecrosis of the knee, and small areas of osteonecrosis of the hip, which may spontaneously heal without treatment. Osteonecrosis heals without treatment in about 80% of people if the disorder is diagnosed early and if the affected area is small.
Spontaneous osteonecrosis of the knee is usually treated without surgery, and pain usually resolves.
Surgical procedures
There are a number of surgical procedures that slow or possibly prevent progression of the disorder. These procedures are done to preserve the joint and are most effective for treating early osteonecrosis, particularly of the hip, that has not yet progressed to bone collapse. If bone collapse has occurred, a type of joint replacement procedure may be done to decrease pain and improve function.
Core decompression, the simplest and most common of these procedures, involves drilling one or many small tracks or holes (perforations) into the area in an attempt to decrease pressure inside the bone. Core decompression often relieves pain and stimulates healing. In about 65% of people, the procedure can delay or prevent the need for total hip replacement. In younger people, core decompression may also be used even if a small amount of collapse already has taken place. The procedure is relatively simple, has a low rate of complications, and requires the use of crutches for about 6 weeks. Most people have satisfactory or good results overall. However, results for any particular person can be hard to predict. About 20 to 35% of people require a total hip replacement.
During core decompression, surgeons may inject a person’s own bone cells into the small hole or holes. This enhancement to the core decompression procedure may help heal the femoral head (which is part of the hip joint).
Bone grafting (transplanting bone from one site to another) is another procedure. For osteonecrosis of the hip, this can involve removing the dead area of bone and replacing it with more normal bone from elsewhere in the body. This graft supports the weakened area of bone and stimulates the body to form new, living bone in the affected area.
An osteotomy is another procedure designed to save the affected joint. This procedure is done particularly in the region of the hip and may be suitable for younger people in whom some degree of collapse already has occurred, which makes them poor candidates for core decompression or other procedures. Usually the osteonecrosis is in the weight-bearing area of the femoral head. An osteotomy changes the position of the bone so that the weight of the body is now supported by a normal area of the femoral head and not by the collapsed area.
Bone grafting and osteotomy are difficult procedures, however, and are not often done in the United States. They require a person to spend up to 6 months on crutches. These procedures are done only at selected centers that have the surgical experience and facilities to achieve the best results.
A total joint replacement is an effective procedure to relieve pain and restore motion if osteonecrosis has caused significant joint collapse and osteoarthritis. About 95% of people benefit from total replacement of the hip or knee (see Hip replacement). With modern techniques and devices, most daily activities can be resumed within 3 months and most joints should last more than 15 to 20 years.
In younger people with osteonecrosis, a total joint replacement may have to be revised (called revision surgery) or replaced at some later time. However, with modern devices, revision surgery has become much less common. Because total joint replacement is now so successful, there is much less need to do other procedures that replace part of the joint or remove the surface cartilage and place a cap on each bone end.
Occasionally, a partial or total replacement of an extremely painful knee or shoulder may be needed for advanced osteonecrosis that is not alleviated by nonsurgical treatment.
More Information
National Institute of Arthritis and Musculoskeletal and Skin Diseases

©Debla2016 Butterfly
The first image at top of page I was given special permission to tweak it for rare disease awareness day
Not all my recipes posted are healthy I do like a good old fashioned dinner or snack now and then but its rare.
I am a patient leader advocate and home cook
I have
Avascular Necrosis-Osteonecrosis From Injury
Osteoarthritis
Inherited Blood Clot Disorder
Hashimoto Thyroiditis
http://avascularnecrosiseducation.com
https://flexitarianforlife.wordpress.com/author/chronicallygratefuldebla/
www.ChronicallyGratefulDebla.com

The real term is Osteonecrosis
What is avascular necrosis-osteonecrosis ?
AVN-ON is a disease that results from the temporary or permanent loss of blood supply to the bone.
When blood supply is cut off, the bone tissue dies and the bone collapses. If it happens near a joint, the joint surface may collapse.
This condition may happen in any bone. It most commonly happens in the ends of a long bone. It may affect one bone, several bones at one time, or different bones at different times.
What causes avascular necrosis?
Avascular necrosis – Osteonecrosis may be the result of the following:
• Injury
• Fracture
• Damage to blood vessels
• Long-term use of medicines, such as corticosteroids
•To many steroid injections
• Excessive, long-term use of alcohol
• Specific chronic medical conditions
What are the risk factors for avascular necrosis-osteonecrosis?
Risk factors include:
• Injury
• Steroid use
• Gaucher disease
• Caisson disease
• Alcohol use
• Blood disorders, such as sickle cell anemia, factor V, eNOS, mthfr, factor viii
• Radiation treatments
• Chemotherapy
• Pancreatitis
• Decompression disease
• Hypercoagulable state
• Hyperlipidemia
• Autoimmune disease
• HIV
• Vasculitis
• Bone Marrow Edema
• Legg Calves Perthes is avn in childhood
Vasculitis
Smoking
High cholesterol
What are the symptoms of avascular necrosis?
The following are the most common symptoms of avascular necrosis. However, each person may experience symptoms differently. Symptoms may include:
• Minimal early joint pain
• Increased joint pain as bone and joint begin to collapse
• Limited range of motion due to pain
The symptoms of avascular necrosis may look like other medical conditions or bone problems. Always talk with your healthcare provider for a diagnosis.
How is avascular necrosis treated?
Specific treatment for avascular necrosis will be determined by your healthcare provider based on:
• Your age, overall health, and medical history
• Extent of the disease
• Location and amount of bone affected
• Underlying cause of the disease
• Your tolerance for specific medicines, procedures, or therapies
• Expectations for the course of the disease
Key points about avascular necrosis
• Avascular necrosis is a disease that results from the temporary or permanent loss of blood supply to the bone. It happens most commonly in the ends of a long bone.
• Avascular necrosis may be the result of injury, use of specific medicines, or alcohol.
• Symptoms may include mild to severe joint pain and limited range of motion.
• Medications,assistive devices, new experimental treatments like Prp and stem cell injections have show great promise but usually not covered by insurance or you may need to have surgery to improve functionality or to stop further damage to the affected bone or joint.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
• Know the reason for your visit and what you want to happen.
• Before your visit, write down questions you want answered.
• Bring someone with you to help you ask questions and remember what your provider tells you.
• At the visit, write down the name of a new diagnosis, and any new medicines, treatments, or tests. Also write down any new instructions your provider gives you.
• Know why a new medicine or treatment is prescribed, and how it will help you. Also know what the side effects are.
• Ask if your condition can be treated in other ways.
• Know why a test or procedure is recommended and what the results could mean.
• Know what to expect if you do not take the medicine or have the test or procedure.
• If you have a follow-up appointment, write down the date, time, and purpose for that visit.
• Know how you can contact your provider if you have questions. You’re physician should always take a few minutes to talk to you and discuss concerns, treatments all treatments not just the ones they do.
If you don’t get good communication you may want to get another opinion and consider changing providers.
Learn to be your own advocate
Your worth it.

Osteonecrosis has many different causes. Loss of blood supply to the bone may lead to bone cell death and can be caused by an injury (bone fracture or joint dislocation; called traumatic osteonecrosis). At times, there may be no history of injury (non-traumatic osteonecrosis); however, other risk factors are associated with the disease such as some medications (steroids, also known as corticosteroids), alcohol usage or blood coagulation disorders. Increased pressure within the bone also is associated with osteonecrosis. One theory is that the pressure within the bone causes the blood vessels to narrow, making it difficult for blood to circulate through the bone. Osteonecrosis can also be associated with other disorders.
The exact reason osteonecrosis develops is not fully understood for some risk factors. Sometimes, osteonecrosis occurs in people with no risk factors (idiopathic).
Some people have multiple risk factors. Osteonecrosis most likely develops because of the combination of factors, possibly including genetic, metabolic, self-imposed (alcohol, smoking), and other diseases that you may have and their treatment.
Injury:
When a joint is injured, as in a meniscus tear, fracture or dislocation, the blood vessels may be damaged. This can interfere with the blood circulation to the bone and lead to trauma-related osteonecrosis. Studies suggest that this type of osteonecrosis may develop in more than 20% of people who dislocate their hip joint. And 15 % of people who have trauma to knee.
Corticosteroid Medications:
Corticosteroids, such as prednisone, are commonly used to treat diseases in which there is inflammation, such as systemic lupus erythematosus, copd, rheumatoid arthritis, inflammatory bowel disease, and vasculitis.
Studies suggest that long-term, high dose systemic (oral or intravenous) corticosteroid use is a major risk factor for non-traumatic osteonecrosis with reports of up to 35 percent of all people with non-traumatic osteonecrosis.
However, there is still some risk of osteonecrosis associated with the infrequent use of corticosteroids, inhaled corticosteroids, or most steroid injections into joints.
Patients should discuss concerns about corticosteroid use with their doctor.
Doctors aren’t sure exactly why the use of corticosteroids sometimes is associated with osteonecrosis. They may have negative effects on different organs and tissues within the body. For example, they may interfere with the body’s ability to build new bones and to break down fatty substances.
These substances would then build up in and clog the blood vessels, causing them to narrow. This then would reduce the ability of blood to flow inside a bone.
Alcohol Use:
Excessive alcohol use is another major risk factor for non-traumatic osteonecrosis. Studies have reported that alcohol accounts for about 30% of all people with non-traumatic osteonecrosis. While alcohol can slow down bone remodeling (the balance between forming new bone and removing bone), it is not known why or how alcohol can trigger osteonecrosis.
Other Risk Factors:
Other risk factors or conditions associated with non-traumatic osteonecrosis include Gaucher disease, pancreatitis, autoimmune disease, cancer, HIV infection, decompression disease (Caisson disease), and blood disorders such as sickle cell disease, factor v, mthfr, and more so always ask your doctor to check you for a clot disorder.
Certain medical treatments including radiation treatments and chemotherapy can cause osteonecrosis. People who have received a kidney or other organ transplant may also have an increased risk.
Osteonecrosis usually affects people between 20 and 50 years of age; about 10,000 to 20,000 people develop osteonecrosis each year in the United States alone.
Osteonecrosis affects both men and women and affects people of all ages. It is most common among people in their thirties and forties. Depending on a person’s risk factors and whether the underlying cause is trauma, it also can affect younger or older people.
After performing a complete physical examination and asking about the patient’s medical history (for example, what health problems the patient has had and for how long), the doctor may use one or more imaging techniques to diagnose osteonecrosis. As with many other diseases, early diagnosis increases the chances of treatment success.
It is likely that the doctor first will recommend an x-ray. X-rays can help identify many causes of joint pain, such as a fracture or arthritis. If the x-ray is normal, the patient may need to have more tests.
Research studies have shown that magnetic resonance imaging (MRI) is currently the most sensitive method for diagnosing osteonecrosis in the early stages. The tests described below may be used to determine the amount of bone affected and how far the disease has progressed.
X-Ray
An x-ray is a common tool that the doctor may use to help diagnose the cause of joint pain. It is a simple way to produce pictures of bones. The x-ray of a person with early osteonecrosis is likely to be normal because x-rays are not sensitive enough to detect the bone changes in the early stages of the disease. X-rays can show bone damage in the later stages, and once the diagnosis is made, they are often used to monitor the course of the condition.
Magnetic Resonance Imaging (MRI)
MRI is a common method for diagnosing osteonecrosis. Unlike x-rays, bone scans, and CT (computed/computerized tomography) scans, MRI detects chemical changes in the bone marrow and can show osteonecrosis in its earliest stages before it is seen on an x-ray. MRI provides the doctor with a picture of the area affected and the bone rebuilding process. In addition, MRI may show diseased areas that are not yet causing any symptoms. An MRI uses a magnetic field and radio waves to produce cross-sectional images of organs and bodily tissues.
Bone Scan
Also known as bone scintigraphy, bone scans should not be used for the diagnosis of osteonecrosis because they may miss 20 to 40% of the bone locations affected.
Computed/Computerized Tomography (CT)
A CT scan is an imaging technique that provides the doctor with a three-dimensional picture of the bone. It also shows “slices” of the bone, making the picture much clearer than x-rays and bone scans. CT scans usually do not detect early osteonecrosis as early as MRI scans but are the best way to show a crack in the bone. Occasionally it may be useful in determining the extent of bone or joint surface collapse.
Biopsy
A biopsy is a surgical procedure in which tissue from the affected bone is removed and studied. It is rarely used for diagnosis, as the other imaging studies are usually sufficiently distinct to make the diagnosis with a high level of confidence.
Treatment
Appropriate treatment for osteonecrosis is necessary to keep joints from collapsing. If untreated, most patients will experience severe pain and limitation in movement within two years. There is no agreed upon optimal treatment for individuals with osteonecrosis.
Early intervention is essential to preserve the joints, but most people are diagnosed late in the disease process.
Several treatments are available that can help prevent further bone and joint damage and reduce pain. To determine the most appropriate treatment, the doctor considers the following aspects of a patient’s disease: the age of the patient; the stage of the disease–early or late; the location and amount of bone affected–a small or large area. The underlying cause has not been shown to influence outcomes of treatment.
The goal in treating osteonecrosis is to improve the patient’s use of the affected joint, stop further damage to the bone, and ensure bone and joint survival. If osteonecrosis is diagnosed early enough, collapse and joint replacement can be prevented. To reach these goals, the doctor may use one or more of the following treatments.
Non-operative Treatment
There is no known pharmaceutical cure for osteonecrosis. Several non-operative treatments have been studied including hyperbaric oxygen therapy, shock wave therapy, electrical stimulation, pharmaceuticals (anticoagulants, bisphosphonates, vasodilators, lipid lowering agents), physiotherapy and muscle strengthening exercises, and combinations thereof. There are conflicting results for some of these treatments, therefore, rigorous, randomized controlled trials with large numbers of patients are still needed to determine the effectiveness of these treatments. Non-operative treatment may be part of a wait-and-see approach based on the size of the area of dead bone. Non-operative treatments cannot be labeled as conservative, since many of them do not slow the progression of the disease or lead to avoidance of a total hip arthroplasty. Most are simply pain-relieving at best.
Reduced weight bearing does not alter the course of the disease and is not a treatment. It may be used to simply permit the patient to better cope with pain until appropriate treatment is instituted.
Surgical Treatment
Core decompression – This surgical procedure removes or drills a tunnel into the area of the affected bone, which reduces pressure within the bone. Core decompression works best in people who are in the earliest stages of osteonecrosis, before the collapse of the dead bone. This procedure sometimes can reduce pain and slow the progression of bone and joint destruction in these patients.
Osteotomy – This surgical procedure reshapes the bone to reduce stress on the affected area. There is a lengthy recovery period, and the patient’s activities are very limited for 3 to 12 months after an osteotomy. This procedure is most effective for patients with advanced osteonecrosis and those with a small area of affected bone.
Bone graft – Bone grafts can be used as part of the surgical treatment for osteonecrosis. Bone grafts can use bone from the same patient or donor bone. Bone graft or synthetic bone graft can be inserted into the hole created by the core decompression procedure. A specialized procedure, called vascularized bone grafting, involves moving a piece of bone from another site (often the fibula, one of the bones of the calf, or the iliac crest, a portion of the pelvic bone) with a vascular attachment. This allows for support of the diseased area as well as a new source of blood supply. This is a complex procedure and is performed by surgeons that are specially trained. Another type of bone grafting, involves scraping out all of the dead bone and replacing it with healthier bone graft, often from other portions of the patient’s skeleton.
A unique type of bone graft involves the use of a patient’s own cells that are capable of making new bone. Often these cells are a type of stem cell from the bone marrow or other bodily tissues. There has been increasing interest in the potential of stem cell therapy. This is also being studied for the treatment of osteonecrosis. Mesenchymal stem cells, which are a type of ‘adult’ stem cell, can grow and develop into many different cell types in the body. Physicians take the patient’s own mesenchymal stem cells (autologous transplant) and place them into the affected bone to stimulate bone repair and regeneration.
Arthroplasty/total joint replacement – Total joint replacement is the treatment of choice in late-stage osteonecrosis when the joint is destroyed. In this surgery, the diseased joint is replaced with artificial parts. It may be recommended for people who are not good candidates for other treatments, such as patients who do not do well with repeated attempts to preserve the joint. Various types of replacements are available, and people should discuss specific needs with their doctor.
For most people with osteonecrosis, treatment is an ongoing process. Doctors may first recommend the least complex and invasive procedure, such as protecting the joint by limiting high impact activities, and watch the effect on the patient’s condition.
Other treatments then may be used to prevent further bone destruction and reduce pain such as core decompression with bone graft/stem cell therapy,Prp injections, A2m injection. But some of these new treatments may not be covered by your insurance.
Eventually patients may need joint replacement if the disease has progressed to collapse of the bone. It is important that patients carefully follow instructions about activity limitations and work closely with their doctor to ensure that appropriate treatments are used.
Scientists, researchers, and physicians continue to pursue a better understanding of how this disease occurs as well as compare the effectiveness of current and newly developed therapies. Often, this requires a clinical trial to answer questions and gain additional knowledge.
Information on current clinical trials is posted on the Internet at www.clinicaltrials.gov. All studies receiving U.S. government funding, and some supported by private industry, are posted on this government web site.
Information
The Many Different Materials Used in Hip Replacement Devices.
If you need a hip replacement it’s best to educate yourself .
Hip replacement devices break into a few big categories:
Metal on Metal (MOM) – These are what they sound like. Both the socket and the ball are made of stainless steel, titanium, chromium, cobalt or some combination of these. One sub-type of a MOM hip is a minimally invasive model which usually is smaller in size, so it can be installed with a smaller incision.
Polyethylene and Metal on Polyethylene (MOP) – Polyethylene is basically plastic, so these hips usually have metal structural pieces and a plastic liner where the ball and socket meet. They can also have a metal ball meeting a plastic socket liner. A sub-type of a polyethylene hip is made with a newer plastic called cross linked polyethylene, which is more durable.
Ceramic on Metal (COM), Ceramic on Ceramic (COC), Ceramic on Polyethylene (COP) – Ceramic hips are made of specialized and more durable versions of the same type of material that plates and bowls are made from. There are ceramic on metal, ceramic on ceramic, and ceramic on polyethylene versions. While these are durable, they can be vulnerable to fracture and breaking under big stresses.
Wear Particles
If for some reason I would need a hip replacement, my single biggest concern would be wear particles. This phenomenon first came to light about 5 – 7 years ago when surgeons began to replace the first worn out or failed metal on metal (MOM) hips. What they found in some patients was scary. Basically, the entire area directly around the hip replacement device had turned into a mass of black goo.
Then studies were published showing that those microscopic metal shavings were leaching into the blood stream and causing elevated metal ion levels. Additional studies began to point out that some people’s tissue was so sensitive to this junk that they formed pseudotumors, which are basically big solid masses of irritated tissues, some of which could press on important nerves. Finally, genetic studies showed that not only was this tissue visibly unhappy, the cells were getting damaged at a genetic level from the wear particles.
When all of this first came to light, it looked like only MOM hips were involved. However, as the research below shows, the issue of wear particles extends to every type of hip made.
ARMD – Adverse Reactions to Metal Debris
Before we begin, it’s worth noting that there is now a name for pissed off tissue caused by wear particles. In a 90s movie, a nuclear war head falls into the wrong hands and the main character is informed that this is called a “Broken Arrow”. He responds to the effect of, “I’m not sure what’s more disturbing, the fact that we just lost a nuclear warhead or that you actually have a name for this”. I feel the same about the fact that the orthopedic joint replacement community now has a name for wear particles that cause problems in patients.
In addition to highlighting research on wear particles, I’ll also look at the durability of each type. So let’s take a look at how to navigate this minefield.
The Research on the Various Types of Hip Replacement Materials – Focused on Wear Particles and Device Failure
MOM or “Metal on Metal”
The “bad boy” of hip replacement types is clearly MOM hips. The funniest thing is that despite all of the absolutely horrific things published about these devices, you can still find Internet ads for many surgeons who will be happy to implant them. They do this by claiming that these are “minimally invasive” hips. While there’s a tiny kernel of truth in that hogwash (the incisions needed to implant them are smaller), there is nothing minimally invasive about amputating a joint and inserting a prosthesis, no matter how you skin that cat. In addition, the smaller the device, the bigger the wear particle issue.
MOM hips produce metal wear particles locally that are then taken up in the bloodstream. In general, smaller MOM hip devices (usually those used for small framed women) have a higher likelihood of producing metal wear particles. This study showed more metal ions in the blood with MOM devices compared to conventional hip replacement prostheses. This randomized trial again demonstrated more metal ions in the blood of women with MOM hips when compared to conventional hip replacement, but also noted that pseudotumors occurred both around these MOM devices and the more conventional MOP devices as well. This recent study showed that metal debris was present in both large and small MOM hip replacement devices.

The latest 2015 consensus guidelines are now not to perform a MOM hip replacement in small women or anybody with a known metal allergy. The latest study on MOM hips and pseudotumors concludes, “Adverse reactions to metal debris in MOM hips may not be as benign as previous reports have suggested.” Not good.
Polyethylene and Metal on Polyethylene (MOP)
When I initially began this literature search, I thought that MOP hips may be better in the wear particle department. After all, you don’t have metal rubbing on metal, but usually metal on plastic. However, I was wrong.
To see how bad things can get with MOP wear particles, I didn’t have to look far. This recent study from 2014 showed an awful side effect of both polyethylene and metal wear particles, a pseudotumor that invaded a woman’s vaginal tissues. This 2015 study was very concerning in that it compared MOP hips to MOM hips with regard to metal levels and chromosome damage in cells. It couldn’t conclude that one was better than the other. Based on this 2014 study, MOP hips wear less, but their wear particles produce slightly more tissue reaction than MOM hips. This is all consistent with a recent study I blogged on, showing that conventional polyethylene wear particles reduced stem cell activity in bone marrow and muscle.
If there is one bright spot in this category, it’s likely the newer highly cross linked polyethylene (HCLP). Based on this recent study, HCLP hips produced fewer wear particles than regular polyethylene. In another study of shoulder replacement devices, the lower debris for these devices was confirmed. In addition, based on this 2014 study HCLP devices seem to withstand unexpected wear and part failure better.
Ceramic on Metal (COM), Ceramic on Ceramic (COC), Ceramic on Polyethylene (COP)
Maybe ceramic is the way to go? After all, what could go wrong with installing a hip replacement device made of the same substance as dinner plates?
This 2015 randomized trial showed that COM hips still regrettably produced metal wear particles that ended up in the blood stream. Some good news for COM hips could be found in this 2015 study. It concluded that while there was swelling around these devices, when compared to minimally invasive MOM hips, there were no pseudotumors seen in COM hips. However, based on this analysis of many studies, there doesn’t seem to be any advantage of COC compared to COP. How does COM and COC compare? Ceramic on metal doesn’t seem to have the same durability as ceramic on ceramic based on this study.
Is Your Surgeon Being Paid to Promote a Certain Type of Hip?
One of the real challenges in navigating this landscape is that regrettably, joint replacement devices have been one of the worst areas of payola in medicine. As reimbursements have declined for the surgical procedures of installing and replacing devices, many surgeons have figured out that they can keep their cash flow stable by taking money from the device manufacturers. This has been the subject of many Department of Justice lawsuits through the years.
The big issue for patients is how to know if their surgeon is recommending a hip device because they really feel that it’s the best, or because they’re getting paid by the company making the device. This Propublica web-site will allow you to research your surgeon’s payment history.
Correct Sizing is Key!
It’s very clear from reviewing the medical research on this topic that a poorly sized hip device is a huge problem for many reasons. First, it will reduce the longevity of the device. Perhaps more importantly, it virtually guarantees more harmful wear particles. And since we’re talking about replacing your hip, a good fit is common sense.
Given the modular nature of these hip devices and the wide array of options, a poor fit should never happen. However, in my experience, hardware fitting issues usually happen when the operating room and/or hospital don’t have the correct size in stock on the day of the surgery. So agree before hand on the size of the components and make sure the staff has double-checked to make sure the hospital has that size in stock.
The upshot? All hip replacement devices produce wear particles. But which is best? It’s clear that when metal on metal implants go bad, things can go very bad with a local tissue reaction that can cause pseudotumors and high metal ions levels in the blood. If I had to get my hip replaced, I would cross this type of implant off my list. Ceramics still produce wear particles and have the added problem of fracturing in an active individual. Polyethylene wear particles in a MOP hip can be just as bad as those from a MOM hip. Given that highly cross linked polythylene has the least wear particles, this is likely the winner. However, realize that not as much is known about tissue reaction to cross linked polyethylene, so that recommendation may change with time. In addition, there are newer types of ceramics that once mated with HCLP could produce less debris.
More information Hip Replacement Material- Regenexx

Avascular necrosis (AVN) develops when a bone loses its blood supply. AVN goes by several other names, including Kummel disease, osteonecrosis, aseptic necrosis, and ischemic bone necrosis. AVN typically affects bone in the hips, thighs, knees and shoulders—although it can develop in any bone in the body.
Kummel disease is a rarely occurring variation of avascular necrosis that can affect the spine’s vertebrae, usually the thoracic spine (mid back) region. There are many different spine-related disorders that can contribute to disrupting a vertebral body’s blood supply, such as infection, osteoporosis, radiation therapy, steroid use, and metastatic spine tumors. Like other organs in the body, bone needs a healthy blood supply to rebuild itself, stay strong and support the spinal column.
Though Kummell disease is rare, researchers believe it’s becoming more prevalent as the aging population grows. People with osteoporosis and older adults are at a greater risk for developing this disorder.
As our population ages, the prevalence of osteoporosis, its most common fragility fracture (vertebral compression fracture), and Kummel disease will increase.
Also if younger and you are diagnosed with osteoporosis your chances are higher to possibly develop Kummel Disease.
text ©Debla2017
AVN has several risk factors, including medical conditions and lifestyle choices that may increase your chances of developing the disorder:
Diagnosing spinal AVN caused by trauma—also called Kummell disease—begins with a thorough review of your medical history and symptoms. This is all part of your physical exam.
After your physical exam, your doctor may order imaging scans to better see changes in your vertebrae.
Below are some of the tools your doctor may use to diagnose Kummell disease:
The goals of treatment for AVN include improving your use of the affected joint, stopping further damage to the bone, and ensuring bone and joint survival.
If you have an early-stage form of Kummell disease, your doctor may prescribe medications to manage pain and/or inflammation. Physical therapy (PT) may be included in your treatment plan. A physical therapist can teach you how to exercise safely to protect your joints and bones while building strength, flexibility and endurance.
Though non-surgical treatments may help keep pain at bay, they are generally a temporary solution for people with Kummel disease. In many cases, spine surgery is necessary to prevent the condition from progressing to a point that it harms your quality of life.
Spine surgery for Kummel disease may have several purposes, depending on your specific symptoms. As such, your surgeon may use a single surgical approach or combine techniques to give you the best possible outcome. For example:
Another surgical option for AVN is known as core decompression. This procedure involves removing the inner layer of bone, which reduces pressure within the bone, increases blood flow to the bone, and allows more blood vessels to form.
Core decompression works best in people who are in the earliest stages of avascular necrosis, often before the collapse of a joint. This procedure may reduce pain and slow progression of bone and joint destruction.
After core decompression, your surgeon may implant bone graft to help stimulate new bone growth and healing. Bone graft transplants healthy bone from a part of the body, such as the leg, to the diseased area. Several synthetic bone grafts are also available. Depending on the location and extent of the surgery, expect a lengthy recovery period, usually from 6 to 12 months.
As with all areas of medicine, researchers are continuously exploring treatments that may help people with AVN. One area of interest is therapies that increase the growth of new bone and blood vessels. These treatments have been used experimentally alone and in combination with other treatments, such as osteotomy and core decompression.
Your doctor will work with you to develop a custom treatment plan that addresses your symptoms and medical history.
For most people with avascular necrosis (also known as osteonecrosis, aseptic necrosis, and ischemic bone necrosis), treatment is an ongoing process. Your doctor may first recommend the least invasive approach and observe how you respond before progressing you to more substantial AVN therapies. If your condition affects your spinal vertebrae and was caused by trauma or injury (Kummell disease), several treatments may help prevent complications like spinal fracture, kyphosis deformity, and nerve pain from disrupting your life.
